Healthcare IT Is Expanding. Continuous Patient Monitoring Still Isn’t
The Hidden Care Gap Remote Patient Monitoring Is Trying to Solve
Reader Note
This piece is written for readers exploring the intersection of healthcare IT, digital health infrastructure, and patient monitoring technologies.
It will be particularly relevant for:
• healthcare IT leaders
• digital health founders
• hospital administrators
• health system strategists
• life sciences professionals
• investors tracking healthcare transformation
The focus here is not simply technology adoption.
It is a deeper system question.
Why does healthcare generate enormous volumes of data yet still struggle to observe patients continuously between visits?
△ ▽ ⧋
Cognitive Index | By Beyond Coordinates
The Healthcare Data Paradox
Healthcare has digitized rapidly over the past two decades. Electronic Health Records (EHRs) now operate across most hospitals in developed markets, while wearables, connected medical devices, and digital health platforms generate increasing volumes of patient data outside clinical environments.
Yet despite this growth, Remote Patient Monitoring systems remain unevenly integrated into everyday clinical practice.
Healthcare today produces close to 30 percent of the world’s data, making it one of the fastest growing information ecosystems of any industry. Despite this expansion, clinicians still face a practical limitation. Once patients leave hospitals or clinics, real-time visibility into patient health often disappears.
Most healthcare systems still operate around periodic clinical encounters, not continuous monitoring. This gap between available health data and actual clinical visibility remains one of the structural challenges in modern healthcare.
Why Healthcare Systems Were Built for Episodic Care
Modern healthcare infrastructure developed around acute medical events. Patients experience symptoms, seek medical attention, receive treatment, and eventually leave the hospital.
Clinical workflows, hospital operations, and most healthcare IT systems were designed to support this sequence. Electronic health records primarily document diagnoses, procedures, and hospital visits rather than continuous patient monitoring.
This model worked when medicine focused largely on infectious disease and surgical care.
Today the dominant challenge is different. Chronic diseases such as cardiovascular illness, diabetes, and respiratory disorders account for more than 70 percent of global healthcare spending. Managing these conditions requires ongoing observation rather than isolated clinical encounters.
The Post Discharge Patient Monitoring Gap
A major visibility gap appears after patients leave clinical supervision. Recovery continues at home, where healthcare providers have limited insight into how conditions are evolving.
Small changes in blood pressure, oxygen levels, or glucose readings may occur days before symptoms become severe enough to require treatment. By the time patients return to hospitals, the condition may already require more intensive care.
This contributes to hospital readmissions, which remain a significant cost driver. In the United States alone, avoidable readmissions are estimated to cost the healthcare system tens of billions of dollars each year.
The challenge is not the absence of health data. The challenge is limited monitoring between clinical visits.
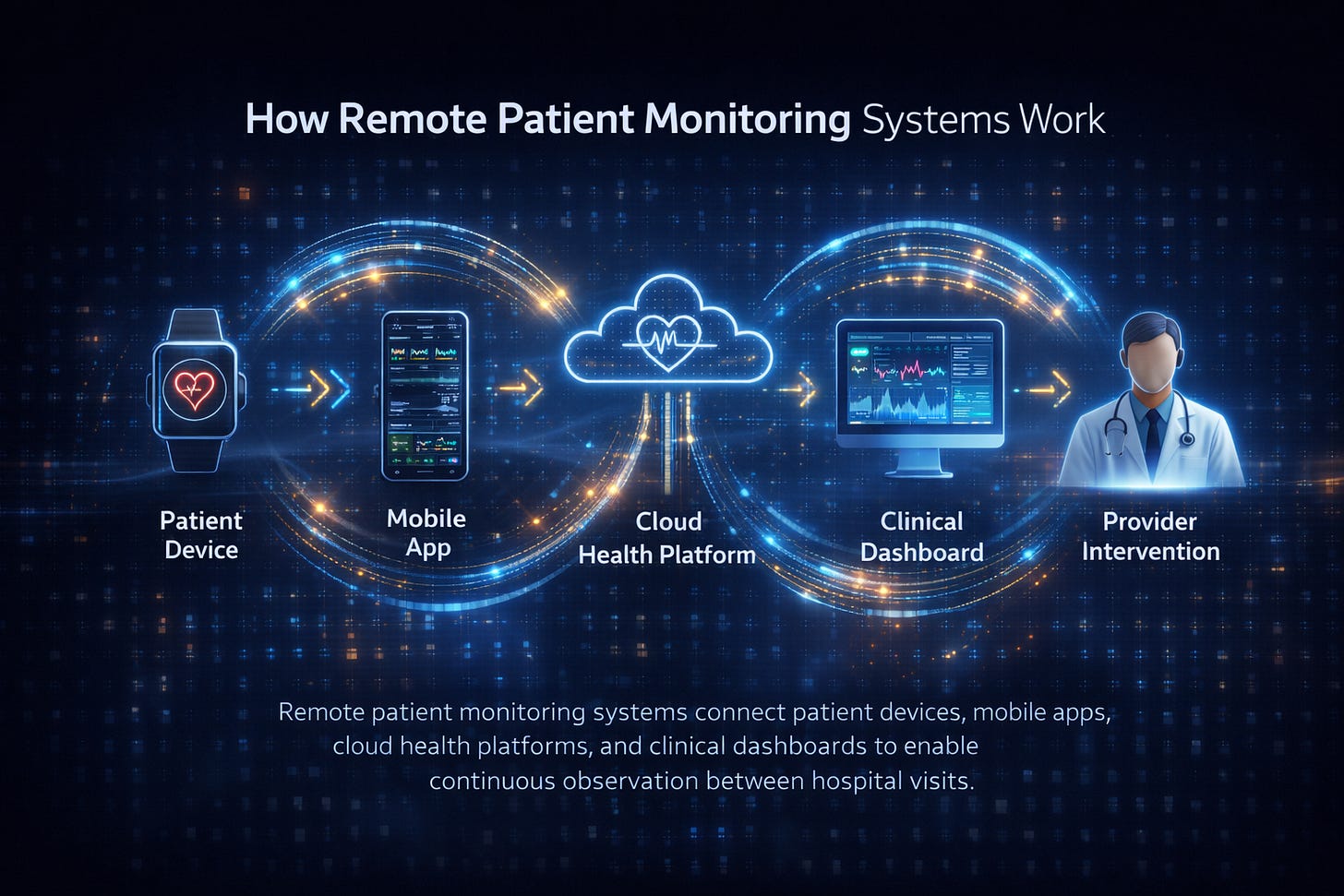
How Remote Patient Monitoring Works
Source: ThoroughCare (YouTube)
Value Based Care and the Economics of Prevention
Healthcare payment models are gradually shifting. Governments and insurers are promoting Value Based Care, a model that links reimbursement to patient outcomes rather than service volume.
Under these models, hospitals are incentivized to reduce readmission rates, improve chronic disease management, and lower long-term treatment costs.
Preventing deterioration therefore becomes financially important.
Technologies that allow clinicians to identify early warning signs can reduce hospital admissions and improve outcomes. Remote monitoring systems support this approach by providing additional clinical information between visits.
Revenue Cycle Management and Digital Health Adoption Challenges
Adopting new healthcare technologies also requires alignment with reimbursement systems.
Hospitals depend on Revenue Cycle Management (RCM) processes to document care and secure payment from insurers. Introducing remote monitoring programs often requires new documentation workflows, billing codes, and compliance procedures.
Healthcare providers must translate remote monitoring activity into reimbursable clinical services.
This requirement slows adoption. Even when technology is effective, implementation depends on whether reimbursement systems support it.
Healthcare innovation therefore advances at two different speeds. Technological capability evolves quickly, while reimbursement infrastructure adapts more gradually.
Remote Patient Monitoring and Continuous Health Data
Remote Patient Monitoring (RPM) systems attempt to close the visibility gap between hospital visits. Connected medical devices and wearable sensors track physiological indicators such as heart rate, blood pressure, oxygen saturation, and glucose levels from a patient’s home.
Home monitoring programs extend clinical observation beyond hospital environments. Platforms developed by companies such as Biofourmis and Current Health provide infrastructure that allows clinicians to review patient data remotely.
These technologies aim to improve clinical visibility between visits, particularly for individuals managing chronic disease or recovering after hospitalization.
The hidden infrastructure behind continuous care
Healthcare IT Integration and Interoperability Challenges
Despite progress in digital health technology, integration remains difficult.
Healthcare IT ecosystems involve hospitals, insurers, device manufacturers, and analytics platforms that often operate on separate systems. Interoperability between healthcare platforms is still inconsistent.
Many Electronic Health Record systems do not integrate easily with external monitoring devices.
Clinicians must also review increasing volumes of incoming patient data. Excessive alerts can lead to alert fatigue, which reduces the effectiveness of monitoring programs.
Healthcare organizations therefore face both technical and operational challenges when integrating remote monitoring into everyday clinical workflows.
Toward Continuous Care Infrastructure
Healthcare delivery is gradually expanding beyond hospitals and clinics.
Remote monitoring technologies, telemedicine platforms, and digital health tools allow providers to follow patients more closely outside traditional clinical settings.
Hospitals remain central to treatment, yet care delivery increasingly includes home monitoring, digital follow-ups, and remote clinical observation.
These changes aim to improve visibility into patient health between visits, particularly for patients managing chronic illness or recovering from hospitalization.
Closing Observation
Healthcare systems now generate large volumes of patient data, yet many providers still lack consistent insight into patient health between visits.
Remote monitoring technologies attempt to address this gap by extending clinical observation beyond hospitals.
Their long-term impact will depend not only on technology but also on how effectively healthcare organizations integrate monitoring systems into everyday clinical practice.
△ ▽ ⧋
Technology expands.
Data multiplies.
Care still waits.
Related Exploration
Conversation
If these ideas intersect with your work or research, thoughtful conversations are always welcome.
hello@beyondcoordinates.com
Authorship note: This article was written and reviewed using RADAR/GLTR authorship analysis tools to verify natural language authenticity.
© Beyond Coordinates, 2026. All rights reserved.